What Happens During a Prostate Biopsy and What to Expect After

Prostate biopsy is one of the most commonly performed urological procedures in the United States, with approximately 1 million performed every year. Yet a growing body of clinical evidence and physician experience suggests that many of those biopsies may be unnecessary, premature, or ordered before less invasive alternatives have been fully explored.
If your doctor has recommended a prostate biopsy, understanding what the procedure actually involves and whether you truly need it right now is the most important first step you can take.
What is a Prostate Biopsy and How is it Done?
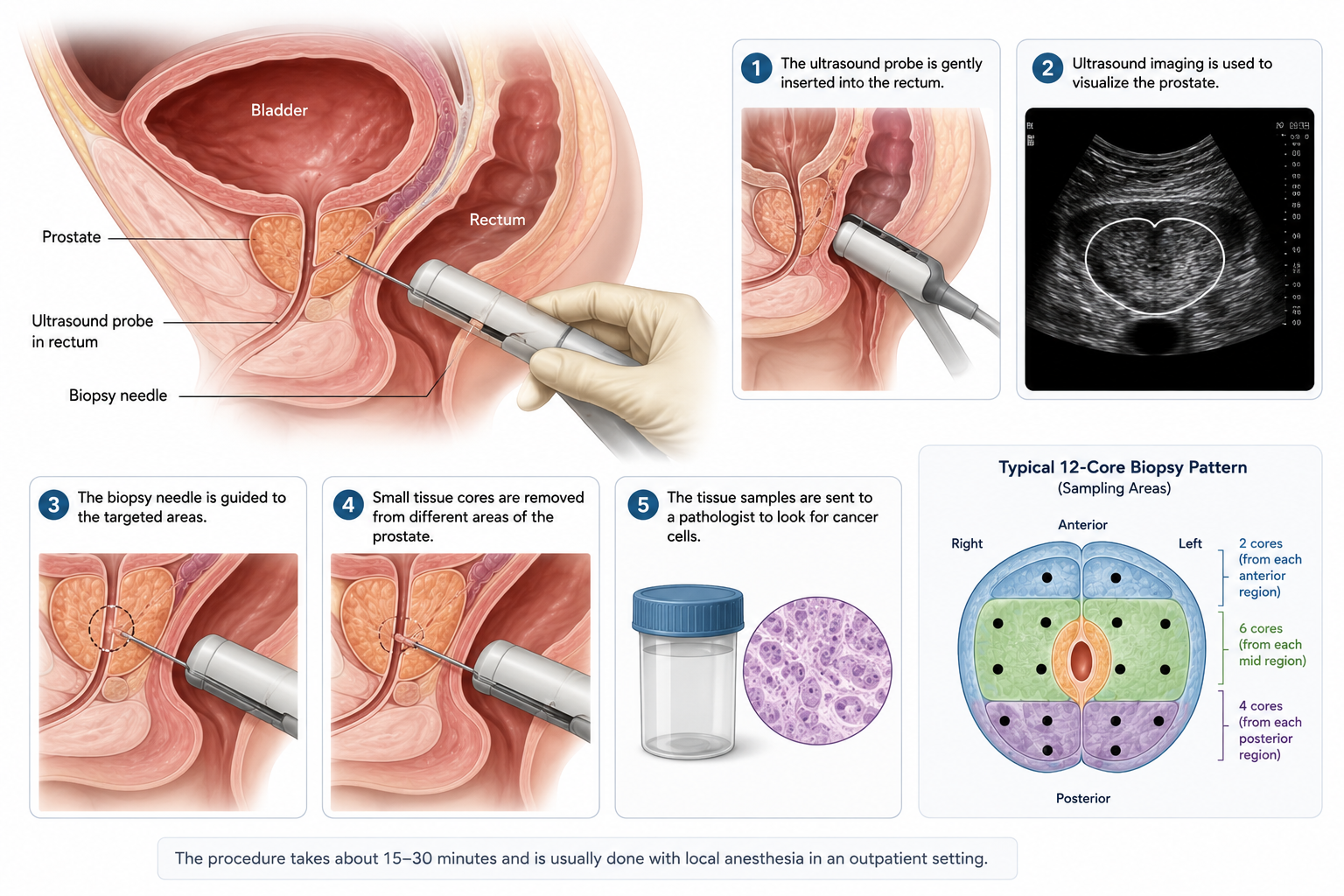
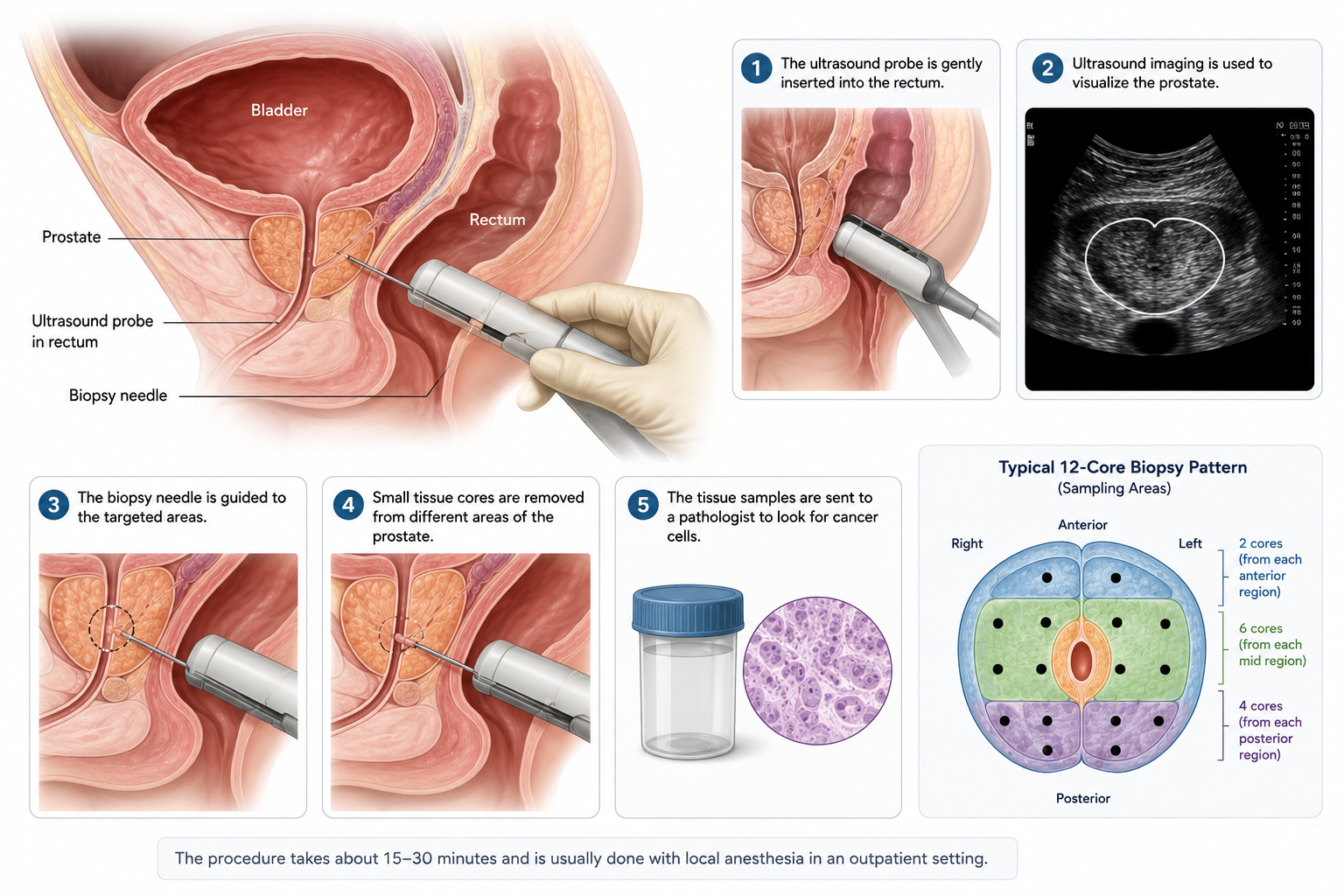
A prostate biopsy is a procedure in which a urologist removes small tissue samples from the prostate gland using a fine needle. Those samples are examined under a microscope to look for cancerous cells. The most common technique is the transrectal ultrasound-guided biopsy, called a TRUS biopsy, in which an ultrasound probe is inserted into the rectum to guide a needle into the prostate. Between 10 and 14 tissue cores are extracted from different regions of the gland, and the whole procedure takes roughly 15 to 30 minutes in an outpatient setting.
Local anesthesia is administered before sampling begins, and most men describe the experience as pressure or brief discomfort rather than sustained pain. A newer technique, the transperineal biopsy, passes the needle through the skin of the perineum rather than the rectal wall and carries a meaningfully lower risk of infection. Your urologist will recommend one approach or the other based on your imaging findings, your anatomy, and their clinical preference.
What the procedure brochure rarely emphasizes is that a biopsy is not a neutral act. It introduces a needle, multiple times, into a gland surrounded by sensitive structures. That carries real consequences, and every man deserves to understand them before signing a consent form.
4 Side Effects of Prostate Biopsy Nobody Prepares You For
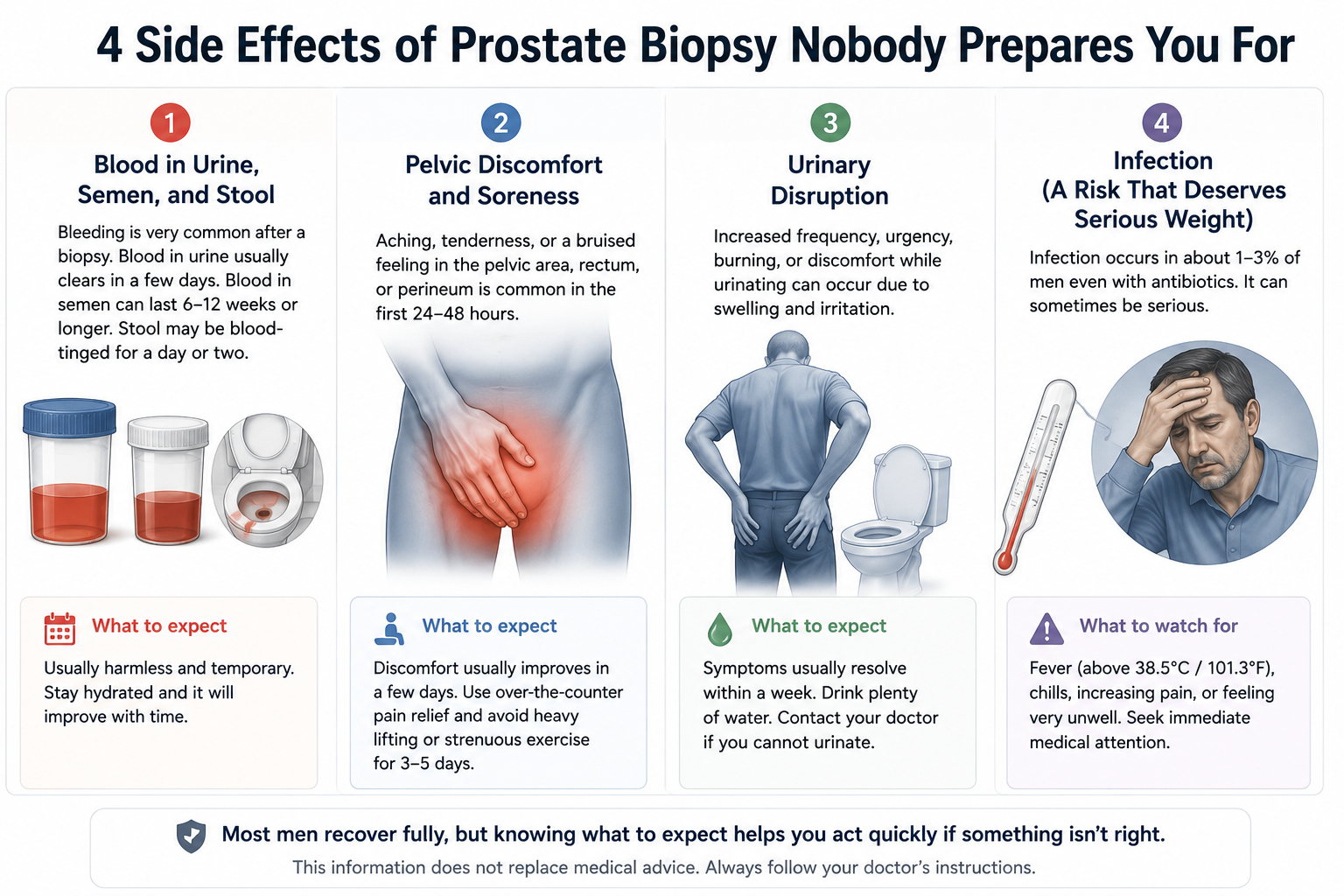
Recovery from a prostate biopsy is presented by many clinics as routine and minor. For a number of men, that description holds. For others, the aftermath is more disruptive than they were led to expect.
These are the four things most likely to occur after the procedure:
- Blood in Urine, Semen, and Stool
Blood in the urine after a biopsy typically clears within a few days. Blood in the semen, however, can persist for six to twelve weeks, and in some men, it lingers for several months. This is a predictable consequence of needle trauma to tissue that has a rich blood supply. Stool may also appear blood-tinged in the first day or two.
Staying well hydrated helps the body clear these signs of trauma more efficiently. Most men find that the persistence of blood in semen is the most psychologically unsettling part of recovery, particularly because it extends so far beyond the procedure itself.
- Pelvic Discomfort and Soreness
Rectal tenderness, pelvic aching, and perineal soreness are common in the 24 to 48 hours following a biopsy. Over-the-counter acetaminophen is usually sufficient to manage it, and most men return to desk work within a day or two. Physically demanding activity, heavy lifting, and vigorous exercise should be avoided for three to five days.
The discomfort is generally described as a bruised sensation rather than sharp pain. If soreness is worsening after the first day instead of gradually improving, that change is a clinical signal worth reporting to your urologist promptly.
- Urinary Disruption
Increased frequency, urgency, and a burning sensation during urination are reported by a meaningful portion of men in the days after a biopsy. These symptoms arise from swelling and irritation near the urethra and typically resolve within a week. Drinking sufficient water dilutes urine and reduces the discomfort.
In rare cases, significant prostate swelling can partially obstruct urinary flow and lead to temporary urinary retention. An inability to urinate at all is not a side effect to manage at home. It requires prompt medical evaluation.
- Infection (A Risk That Deserves Serious Weight)
Infection is the most clinically significant complication of a prostate biopsy, and it occurs in approximately 1% to 3% of cases even when prophylactic antibiotics are prescribed. The warning signs are fever above 38.5 degrees Celsius, chills, significant pelvic pain, and a general sense of being seriously unwell in the two to five days after the procedure.
These symptoms require immediate medical evaluation rather than watchful waiting at home. In rare instances, sepsis can develop rapidly, and it responds far better to treatment when caught early. This is not a theoretical risk. It is the reason physicians set a specific fever threshold for patients before they leave the clinic.
What a Prostate Biopsy Cannot Tell You
A negative biopsy result, meaning no cancer found in the sampled tissue, offers reassurance but not certainty. The needle samples only a fraction of the prostate's total volume. Cancer can be present in regions that were not sampled, which is why physicians sometimes recommend repeat biopsies when clinical suspicion remains elevated despite a clear result. A positive result will include a Gleason score, a grading system that describes how aggressive the cancer cells appear. Lower scores suggest a slower-growing disease. Higher scores indicate cells with more significant alterations.
What a biopsy cannot tell you is whether the cancer it finds, if any, will ever cause you harm. That distinction sits at the center of one of the most important conversations in modern prostate cancer medicine.
How to Approach the Conversation with Your Doctor

Before agreeing to a biopsy, there are questions you should ask your urologist directly:
- How significantly elevated is my PSA, and has it been rising over time or remaining stable?
- Has an MRI been considered or performed?
- What would a positive result at my PSA level most likely mean for my treatment options?
- Are there monitoring approaches that would preserve the option for later biopsy without a meaningful clinical cost?
A physician who welcomes those questions is practicing the kind of medicine that serves patients well. A physician who cannot explain why the biopsy is necessary right now, rather than after further evaluation, is worth getting a second opinion from.
Frequently Asked Questions
How long does a prostate biopsy take?
The procedure itself takes 15 to 30 minutes. Most men are in and out of the clinic within an hour, including preparation and a brief post-procedure observation.
Is a prostate biopsy painful?
Most men describe it as uncomfortable rather than acutely painful. Local anesthesia is used, and the majority of patients find it more manageable than anticipated. The recovery period is often the more disruptive part of the experience.
When should I contact my doctor after a biopsy?
Contact your urologist immediately if you develop a fever above 38.5 degrees Celsius, are unable to urinate, or notice that pain is increasing rather than subsiding after the first day.
What if I want to wait before agreeing to a biopsy?
That is a clinically reasonable position in many situations. Ask your physician about PSA trends, MRI findings, and active surveillance as alternatives to immediate tissue sampling.
What does a negative biopsy result mean?
No cancer was found in the sampled tissue. Your physician will advise whether ongoing PSA monitoring remains appropriate based on your individual risk profile and the reason for the original referral.
The Takeaway
A prostate biopsy is a medical procedure with real risks, real side effects, and real limitations in what it can definitively tell you. Understanding those facts does not make you a difficult patient. It makes you an informed one.
One thing that Intellectual Medicine will always stand for is the fact that living longer and living well are not competing values. We believe that no man should feel that agreeing to a procedure is the only responsible path forward. The evidence should lead the decision, and that evidence deserves time, scrutiny, and the right questions before any needle is introduced.
Ready to take the next step? Schedule your one-on-one consultation with Dr. Stephen Petteruti
Get exclusive insights every month
We hate SPAM. We will never sell your information, for any reason.

